You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Throughout the five or so centuries in which complete dentures have been used to replace missing teeth, denture materials have gradually evolved, with modern acrylics becoming predominant in the 20th century. However, the basic procedures used by dental laboratories to create complete dentures have remained relatively unchanged for many decades. Even today, although dental schools are placing less emphasis on denture-fabrication techniques and requiring students to complete fewer complete denture cases, a majority of dental schools still teach the five-appointment denture protocol.1
The advent of modern computer-aided design/computer-aided manufacturing (CAD/CAM) techniques has finally begun to change the process of making dentures.2 Well established in the production of crown-and-bridge and implant-supported prostheses,3,4 CAD/CAM technology has recently been extended to the fabrication of so-called “digital dentures.” At the heart of this approach is the use of three-dimensional (3D) computer software to model the dentures, rather than relying on manual fabrication of a base plate and occlusion rims into which a dental technician manually sets denture teeth. Instead, the 3D modeling software uses algorithms to combine clinical information supplied by the dentist with anthropometric data gathered from a large cross-section of patients.5 All of this information is used to identify incisal edge position, lip support, and midline. Using rapid-prototyping technology, a prototype of the 3D denture model can then be printed, tried in, and adjusted if necessary. Fabrication of the final denture is then based on the perfected try-in.
There are now several digital denture systems available to choose from, such as AvaDent Digital Dentures (Global Dental Science); DENTCA CAD/CAM Denture (DENTCA, Inc.); and the Pala Digital Denture System (Heraeus Kulzer), in addition to digital design systems, such as Denture Design™ (3Shape). Digital denture processes make it possible to create better-fitting dentures in significantly less time. Instead of the five visits typically required by the conventional denture-making process, digital dentures commonly require only two or three visits. Chairtime can be slashed from 5 or more hours to about 1 hour, with average processing time dropping from 30 days to about 10 days.
Whether fabricated conventionally or digitally, success with all dentures begins with making highly accurate impressions, a task that can pose significant challenges for many dentists.6 Bite registration, too, can be vexing.
The Pala Digital Denture system combines both these tasks and simplifies them. Rather than scheduling separate appointments to make the impressions and capture the jaw relation, the clinician can accomplish both in a single appointment. This is accomplished using segmented impression trays that have a slot assembly designed to support a central bearing device—a well-proven method for obtaining centric relation (CR) bite records.7,8 Trays of four sizes come included with the digital denture kit, along with scannable polyvinyl siloxane impression materials, bite-registration materials, and complete clinical support documentation.9 Once a tray has been selected that best matches a given edentulous arch form, it can be modified both with heat and/or by removing any excess tray material with a lab bur.
The impressions and other clinical documentation are sent to the local laboratory for scanning. Next, the scan files are digitally sent to the Heraeus Pala center, along with photographs and a complete checklist of clinical documentation. At the processing center, all the data is used to develop the denture design, from which a stereolithographic prototype is printed. This is returned to the dentist for a traditional denture try-in appointment. After the try-in is adjusted, if necessary, and approved, the final denture is manufactured at the Heraeus Pala center, using a proprietary process.
The following case report illustrates fabrication of complete upper and lower dentures using the Heraeus Kulzer Pala Digital Denture protocol.
Case Report
The patient was a 55-year-old woman who had experienced a number of illnesses, including cancer, for which she had been treated 10 years earlier. After consulting with her physicians, a determination was made that there were no current contraindications for dental treatment.
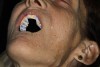
Clinical examination revealed that her maxillary denture fit poorly, in addition to being unesthetic. Her six remaining mandibular teeth and root tips were unsalvageable (Figure 1). The patient’s perioral musculature was noted to be highly mobile. Furthermore, photographs taken when she was in her mid-20s indicated that her original dentition showed maxillary excess, resulting in a “gummy” smile (Figure 2). Discussion with the patient revealed that her treatment expectations were reasonable. She provided informed consent to a treatment plan that called for extraction of her remaining mandibular teeth, followed by fabrication of new complete dentures for both arches, using a digital denture protocol.
The teeth were extracted, and after 8 weeks, the patient returned to begin the denture-development process. The overall size of the patient’s edentulous arches was assessed, and segmented impression trays were selected from the Pala denture kit to fit them. The kit also includes a papillameter and a jaw gauge. Measurements taken with them are used in conjunction with the other clinical data in the computer algorithm.
To develop border moulding and establish stable stops for a final wash impression, initial maxillary (Figure 3) and mandibular impressions were taken, using the scannable polyvinyl siloxane impression material. The clinical reference guide that comes with the denture kit includes detailed instructions for the impression-development process. Evaluation of the initial impressions revealed a few minor impingements on the intaglio surfaces.
After some slight modification of the initial impressions and tray borders to adjust the tissue impingements, wash impressions were made with light-body impression material. The mandibular retromolar pads and maxillary hamular notch areas were then separated from the impression trays, using a scalpel to cut along a line built into the trays. The posterior areas of the trays were removed to ensure that the bite could be registered without any posterior interference.
The central bearing device included in the kit was then fit into the tray slots. The mandibular adjustable guide pin was used to establish vertical dimension of occlusion (VDO) and to serve as a stylus against the fixed plate built into the upper impression tray.
The truncated trays with their respective central bearing device components were inserted in the patient’s mouth. The central bearing device was set at the desired vertical dimension, using the adjustable guide pin. Vertical dimension was determined through comparison with preexisting VDO and evaluation of lip posture and facial profile.
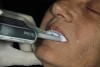
The patient was then instructed to go through protrusive and lateral excursions. A self-adhesive inked sheet is included in the kit; it leaves the distinctive “crow’s foot” range of mandibular motion, with the point of the foot marking defined as CR (Figure 4). A small dimple was cut at that point to stabilize jaw position by holding the guide pin in a repeatable reference position.
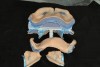
Using sufficient material to stabilize the trays, bite-registration material was injected to record the inter-jaw relationship (Figure 5 through Figure 8). Clinical information checklists were completed, and along with patient photography, the package was sent to the dental laboratory. There the entire impression tray and bite-registration assembly were scanned, and the scan data and other materials were transmitted electronically to the Pala Denture Processing Center.
At the processing center, a try-in denture was designed, based on the information provided for this specific patient. A prototype of the denture was made using 3D printing, and approximately 10 days after the impression appointment, the try-in denture was sent back to the dentist to be evaluated clinically.
The patient had been forewarned that the try-in denture would be monochromatic (Figure 9). Although its extremely white appearance and the absence of any colored gingival tissue can be off-putting to some, this particular patient adjusted to it readily. When it was tried in the patient’s mouth, the basal seat and occlusion were judged to be excellent. However, the central incisors required minor lengthening. These changes were requested via e-mail, supplemented by photograph and a feedback checklist. Had more extensive changes been necessary, new impressions of one or both arches could have been taken, along with new bite registrations. The try-in denture could have been sent back for modification, or a new one could have been fabricated before development of the final appliance.
About 2 weeks later, the patient returned for delivery of the final dentures. Upon their insertion, a satisfying sound of suction was noted for both arches. The basal seat was evaluated, and both dentures appeared very stable. Pressure-indicating paste revealed no pressure spots. The occlusion was evaluated both visually and with articulating paper. Contacts were equal and well distributed. The patient had never worn a lower denture, and some slight lisping was noted during assessment of the phonetics. But this was minor, and at the 3-day recall appointment, it had virtually disappeared.
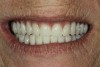
As for the esthetics, the patient’s mobile musculature and maxillary excess did result in a somewhat “gummy” smile, but the patient was enthusiastic about both her appearance and high level of comfort (Figure 10 and Figure 11).
At the 3-day re-care appointment, one small sore spot was adjusted. The patient continued to express complete satisfaction with the experience. The basal seat of the dentures was considered exceptional, occlusion was stable, and the esthetics were deemed extraordinarily good.
Discussion
A digital approach similar to the one illustrated by this case study may represent the future of complete denture prosthetics. The clinical technique, simplified yet accurate, is easily learned and implemented. It eliminates at least two of the traditional appointment steps in clinical denture fabrication, along with many of the associated techniques.
This development comes at a critical time. The number of adults who need full dentures is increasing; it has been projected to reach 37.9 million adults by 2020.10 At the same time, denture patients can be difficult to please and often have unreasonable expectations.11,12 Many dentists lack confidence in their clinical proficiency and are choosing not to treat fully edentulous patients because they worry about achieving predictable outcomes.13 Further adding to the problems associated with providing dentures to patients who need them is a shortage of qualified, experienced denture laboratory technicians.14 Several laboratory technology programs have closed across the United States, and among those technicians best qualified to produce dentures, the average age is more than 50.15
Conclusion
The ability to fabricate digital dentures solves many of the contemporary challenges posted by the traditional denture-fabrication protocol. A simplified clinical technique that is easy to learn and understand and delivers predictable results will appeal to many dentists. The accuracy of dentures fabricated with CAD/CAM technology and proprietary processing techniques eliminates polymerization shrinkage and subsequent issues with the occlusion and fit of appliances. This workflow may well prove to reduce the need for skilled technicians, provide confidence for clinicians, and generally streamline the entire denture-fabrication process.
References
1. Petropoulos VC, Rashedi B. Complete denture education in U.S. dental schools. J Prosthodont. 2005;14(3):191-197.
2. Lozada JL, Garbacea A, Goodacre CJ, Kattadiyil MT. Use of a digitally planned and fabricated mandibular complete denture for easy conversion to an immediately loaded provisional fixed complete denture. Part 1. Planning and surgical phase. Int J Prosthodont. 2014;27(5):417-421.
3. Duret F, Blouin J-L, Duret B. CAD/CAM in dentistry. J Am Dent Assoc. 1988;117:715-720.
4. Cohen A. Digital technology and the future of dentistry using cutting edge production methods to create industry leading restorations. Inside Dent Tech. 2013;4(10):72-73.
5. Sawiris MM. The role of anthropometric measurements in the design of complete dentures. J Dent. 1977;5(2):141-148.
6. Duncan JP, Taylor TD. Teaching an abbreviated impression technique for complete dentures in an undergraduate dental curriculum. J Prosthet Dent. 2001;85(2):121-125.
7. El-Gheriani AS, Winstanley RB. The value of the Gothic arch tracing in the positioning of denture teeth. J Oral Rehabil. 1988;15(4);367-371.
8. Massad JJ, Connelly ME, Rudd KD, Cagna DR. Occlusal device for diagnostic evaluation of maxillomandibular relationships in edentulous patients: a clinical technique. J Prosthet Dent. 2004;91(6):586-590.
9. Drago CJ. A retrospective comparison of two definitive impression techniques and their associated postinsertion adjustments in complete denture prosthodontics. J Prosthodont. 2003;12(3):192-197.
10. Douglass CW, Shih A, Ostry L. Will there be a need for complete dentures in the United States in 2020? J Prosthet Dent. 2002;87(1):5-8.
11. Beck CB, Bates JF, Basker RM, et al. A survey of the dissatisfied denture patient. Eur J Prosthodont Restor Dent. 1993;2(2):73-78.
12. Yoshizumi D. An evaluation of the factors pertinent to the success of a complete denture service. J Prosthet Dent. 1964;14(5):866-878.
13. Holt LS. Digital dentures are a reality: a case study. Inside Dent. 2015;11(Spec ed 1);2-5.
14. Christensen G, Yancey WR, Schoenbaum TR. The mounting challenges facing the lab industry and the effects on clinical practice. Dental Economics. 2013;103:36-39.
15. Zamanian K, Wong J. New technologies guide paradigm shifts in dental prosthetics industry. Business USA. Jan. 30, 2012. Dental Tribune website. http://www.dental-tribune.com/articles/business/usa/7335_new_technologies_guide_paradigm_shifts_in_dental_prosthetics_industries.html. Accessed February 2, 2015.