You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Over the past 30 years, significant progress has been made in the prevention of dental caries in children and adolescents. While caries has decreased on interproximal surfaces, occlusal pit and fissure caries have increased.1,2 In general, research has demonstrated that caries on occlusal and buccal/lingual surfaces account for almost 90% of caries experienced in children and adolescents.3 The reason for this high rate of caries relates specifically to the pit and fissure morphology of occlusal and buccal/lingual surfaces that are not affected by the caries-preventive effects of systemic and topical fluorides.
As part of a comprehensive preventive care, dental sealant application supplements regular oral hygiene practices and dental examinations. Sealants are the most effective clinical technique to prevent pit and fissure caries. The cost effectiveness of sealants, naturally, is based upon sealant retention. While the rates of sealant retention on occlusal surfaces are relatively high at 5 years,4-7 sealant retention for buccal and lingual pits and fissures of molars is considerably lower.8 While there is a desire to seal all at-risk teeth, the question arises of how to handle difficult-to-seal teeth such as the partially erupted dentition.9 When comparing retention of sealants on at-risk teeth that were fully erupted to those that were partially erupted at 3 years after sealant placement, it was found that no replacement of sealants was necessary for the fully erupted, sealed teeth while teeth with gingival tissue at the level of the distal marginal ridge had a 26% sealant replacement rate. Isolation of the tooth and access to the pits and fissures contribute to sealant success. Teeth should therefore be more fully erupted into the oral cavity before attempting the placement of a resin sealant.
Morphology and Prevention
Using a dental mirror and explorer and a dry tooth during a clinical examination helps with the decision whether an occlusal surface of a permanent molar or premolar needs a sealant or restoration. Pits and fissures have variations in their appearance in cross section: V-type, U-type, and I-type pits and fissures.10 In most cases the shape of the pit or fissure is such that it is impossible to clean, explaining the high susceptibility of pits and fissures to dental caries.
Why Sealants
In the 1960s, Buonocore and coworkers investigated the use of adhesives to seal caries-susceptible pits and fissures.11,12 By the late 1970s and early 1980s the clinical data on sealants and caries prevention was very positive. Studies have continued to demonstrate sealant success. One 4-year study showed an overall 43% decrease in the prevalence of caries effectiveness with a significantly better sealant retention on premolars (84%) than molars (30%).4 A 7-year study reported 66% complete sealant retention and 14% partial retention.5 Sealant loss was 20% while there was a 55% reduction in caries rate for the sealed teeth versus the unsealed teeth. One 10-year study showed that for over 8,000 sealants placed on permanent first molars, there was 41% complete sealant retention at 10 years and a 58%–63% retention rate over 7 to 9 years.6
The studies show that sealants work if applied correctly. Sealant success is multifactorial.7,13 Technique, fissure morphology, and the characteristics of the sealant contribute to clinical success.14 When one reviews published sealant data, a basic concept of 5%–10% of sealant loss per year has been seen demonstrated.15 This data reveal the importance of reevaluating teeth with sealants on a periodic basis and to reapply if necessary. The one negative aspect of sealants in the realm of dental prevention would be the failure of clinicians to reevaluate and reapply sealants that are lost or failing. Failure to maintain sealants will lead to pits and fissures that were sealed becoming susceptible to bacterial invasion with the need for more invasive tooth preparations and restorations.15 Table 1 lists considerations to be evaluated for early sealant failure.
Based upon the data reported in the aforementioned clinical research reports, it is important that patients with sealants have periodic re-evaluations and reapplication of sealant if necessary. When a sealant needs to be repaired or reapplied, the tooth should be treated as if an initial sealant were to be placed.16
Identifying Teeth to be Sealed
Deciding which teeth are at risk will vary from clinician to clinician and be based upon experience. A possible criterion that may be used is the determination of whether the tooth has deep occlusal pits and fissures. Some concern has been raised with regard to sealing over undiagnosed, incipient carious lesions on the occlusal surface. Research has shown that sealing active caries in pits and fissures from clinical and radiographic findings that there is no progression of the carious lesions.17-19 Therefore, based upon the evidence to date, placing sealants on at-risk teeth is a cost-effective technique while sealant placement over active or incipient carious lesions does not appear to be detrimental.
Types of Sealants
Sealant materials can be classified in various ways, but the most common classification scheme is on the basis of composition. Currently there are two basic sealant types: resin and glass ionomer. This article focuses on resin-based sealants because most of the research data supports their clinical use. The published literature has indicated that clinical retention of resin-based sealants is superior to that of glass ionomer-based sealants.20
Resin-based sealants can be classified in a number of different ways, typically polymerization method, filled or unfilled, colored or clear, color-changing upon polymerization, and moisture tolerant. While there are certain differences in the properties of the cured resins and in clinical technique when using these two classes of material, both self-cure and light-cure sealants appear to provide equivalent clinical effectiveness when applied to etched dry enamel.4-7 Likewise, sealants can also be clear or colored, the latter offering the advantage of visual confirmation of the presence or absence of sealant on a tooth surface.
Clinical Technique
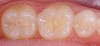
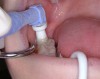
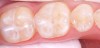
First, examine and evaluate the occlusal surfaces to be considered (Figure 1). Once a diagnosis has been made and it has been determined that a sealant is to be placed, the tooth must be isolated. Isolation of the field can be accomplished with a dental dam or by using absorbents that are frequently changed between steps. Once the tooth (or teeth) have been isolated, the tooth surfaces must be cleaned (Figure 2). The adhesion of sealant to enamel surfaces can be enhanced by cleaning the occlusal surfaces with a non-fluoride, pumice prophylaxis paste or by using an air abrasion device. The surfaces of the teeth are then thoroughly rinsed with an air–water spray and dried.
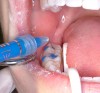
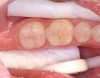
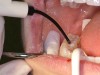
Next, the tooth is etched for 15-30 seconds with a phosphoric acid etchant (Figure 3). Enamel etching is self-limiting in the depth of etchant penetration. Never etch the enamel beyond 60 seconds. The etchant is thoroughly rinsed from the tooth (teeth) with either a water spray or an air–water spray for 10 seconds, then surfaces are completely dried. The enamel surface will have a dull, frosted appearance (Figure 4). If using absorbents such as cotton rolls or blotter paper (Dri-Angle®, Dental Health Products, www.dhpinc.com), change to fresh, dry absorbents.
Sealant is then applied to the occlusal surface with either an applicator tip (Figure 5) or by using a brush type applicator (Figure 6). The sealant should be placed to cover all pits and fissures and to extend onto the cusp ridges. The final sealant thickness upon application should be at least 0.3 mm. This improves the longevity of the sealant.
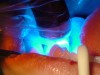
For this case, a light-cured sealant was used (Figure 7). In order to light cure the sealant, there must be sufficient energy to harden the resin sealant. The light must be providing at least 600 mW/cm2 from its tip; the tip of the light must be free of cured resin and not be broken to make sure that sufficient energy is light curing the sealant. It is critical that the curing light be placed within 1 mm of the tooth’s occlusal surface, at right angles to the tooth, and the sealant be cured at least 10 seconds. The light probe must cover the entire occlusal surface. If the diameter of the light probe is too narrow, light cure the mesial first for 10 seconds and the distal for an additional 10 seconds. The sealant is then evaluated for retention and seal of the occlusal surfaces (Figure 8).
Conclusions
Sealants are a highly effective preventive measure for reducing pit and fissure caries. Although recently concern has been expressed related to Bisphenol A (BPA) exposure, the American Association of Pediatric Dentistry’s Guidelines reiterates that the US Food and Drug Administration (FDA) and the American Dental Association (ADA) have concluded that the low level of BPA exposure from dental sealants poses no known health risk.20 A comprehensive review of the dental literature21 concluded from this examination of peer-reviewed publications that sealants are safe, effective, and underused in the United States.
References
1. Eccles MFW. The problem of occlusal caries and its current management. N Z Dent J. 1989;85(380):50-55.
2. Bohannan HM. Caries distribution and the case for sealants. J Public Health Dent. 1983; 43(3):200-204.
3. Ripa LW, Leske GS, Sposato A. The surface-specific caries pattern of participants in a school-based fluoride mouthrinsing program with implications for the use of sealants. J Public Health Dent. 1985;45(2):90-94.
4. Going RE, Haugh LD, Grainger DA Conti AJ. Four-year clinical evaluation of pit and fissure sealant. J Am Dent Assoc. 1977;95(5):972-981.
5. Mertz-Fairhurst EJ, Fairhurst CW, Williams JE, Della Giustina VE, Brooks JD. A comparative clinical study of two pit and fissure sealants: 7-year results in Augusta, Georgia. J Am Dent Assoc. 1984;109(2):252-255.
6. Romcke RG, Lewis DW, Maze BD, Vickerson RA. Retention and maintenance of fissure sealants over 10 years. J Can Dent Assoc. 1990;56(3):235-237.
7. Simonsen RJ. Retention and effectiveness of a single application of white sealant after 10 years. J Am Dent Assoc. 1987115(1):31-36.
8. Barrie AM, Stephan KW, Kay EJ. Fissure sealant retention: a comparison of three sealant types under field conditions. Community Dental Health. 1990;7(3):273-277.
9. Dennison JB, Straffon LH, More FG. Evaluating tooth eruption on sealant efficacy. J Am Dent Assoc. 1990;121(5):610-614.
10. Nagano T. The form of pits and fissure and the primary lesion of caries. Dent Abstr. 1961;Abstract 6:426.
11. Gwinnett AJ, Buonocore MG. Adhesives and caries prevention. A preliminary report. Br Dent J. 1965;119:77-80.
12. Cueto EI, Buonocore MG. Sealing pits and fissures with an adhesive resin. Its use in caries prevention. J Am Dent Assoc. 1967;75(1):121-128.
13. Simonsen RJ. Retention and effectiveness of dental sealant after 15 years. J Am Dent Assoc. 1991;122(10):34-42.
14. Seleeman JB, Owens BM, Johnson WW. Effect of preparation technique, fissure morphology, and material characteristics on the in vitro margin permeability and penetrability of pit and fissure sealants. Pediatr Dent. 2007; 29(4):308-314.
15. Feigal RJ. Sealants and preventive restorations: review of effectiveness and clinical changes for improvement. Pediatric Dent.1998;20(2):85-92.
16. Srinivasan V, Deery C, Nugent Z. In-vitro microleakage of repaired fissure sealants: a randomized, controlled trial. Int J Paediatr Dent. 2005;15(1):51-60.
17. Handelman Sl, Washburn F, Wopperer P. Two-year report of sealant effect on bacteria in dental caries. J Am Dent Assoc. 1976;93(15):967-970.
18. Jeronimus DJ, Till MJ, Sveen OB. Reduced viability of microorganisms under dental sealants. ASDC J Dent Child. 1975;42(4):275-280.
19. Going RE, Loesche WJ, Grainger DA, Syed SA. The viability of microorganisms in carious lesions five years after covering with a fissure sealant. J Am Dent Assoc. 1978;97(3):455-462.
20. American Academy of Pediatric Dentistry. Guideline on Pediatric Restorative Dentistry. www.aapd.org/assets/1/7/G_Restorative.pdf. Accessed September 3, 2012.
21. Simonsen RJ. Pit and fissure sealant: review of the literature. Pediatr Dent. 2002;24(5):393-414.
About the Author
Howard E. Strassler, DMD
Professor, Department of Endodontics, Prosthodontics, and Operative Dentistry
University of Maryland Dental School
Baltimore, Maryland