You must be signed in to read the rest of this article.
Registration on CDEWorld is free. You may also login to CDEWorld with your DentalAegis.com account.
Diode lasers were approved for surgical use by the Food and Drug Administration in 1996.1 In practice, they are part of a family of near-infrared (invisible) lasers, the original of which was the neodymium-yttrium-aluminum-garnet (Nd:YAG) laser introduced about 6 years before the first diode laser.1 The near-infrared group emit a wavelength of invisible light, or electromagnetic radiation, from 800 to 1,400 nanometers (nm). The diode family of lasers is by far the most prevalent group of devices in the dental laser market. Practitioners have found these units practical, easy to learn and use, and affordable. Dentists have learned to use these devices to effectively prepare soft tissue for impressions, reduce bacteria in infected periodontal pockets, and perform simple and sometimes complex oral surgical procedures. This article will highlight some simple surgical cases.
Diode Laser Science
The diode laser produces invisible light energy. This energy takes the form of coherent light focused on a small spot that concentrates the beam, which is capable of making surgical incisions and excisions.2
The energy is directed into a fiber-optic cable and then into a handpiece and aimed at the target tissue. The fiber-optic cable is usually in light contact with soft tissue for surgery and not in contact when the beam is intended to treat damaged tissue. In surgical mode, the laser beam creates an incision by ablating or vaporizing the target tissue approximately 50% wider than the diameter of the fiber (200 to 400 μm).3 The depth of vaporization is a function of the wavelength, the power of the beam (watts), and the speed of fiber movement in the incision. Typically, the depth of the incision will approximate 200 to 300 μm per single pass with a power of around 1 watt.3
The diode laser beam can be "on" all the time (continuous wave), or it may be pulsed in various ways. Traditional devices have been pulsed with a physical device (gated) and may be controlled by pulsing to a certain percentage of the continuous wave, such as 50% or 25%. The purpose of the pulsing is to yield more control to the operator in avoiding undesirable thermal effects, such as charring of the lased and adjacent tissue. Overheating tissue is contraindicated because it may cause unintentional postoperative pain and shrinkage of the remaining tissue. Newer devices have been introduced that emit a superpulsed beam. The advantages of these devices are faster ablation with less lateral thermal damage to the adjoining tissue.4
A diode laser beam, as well as other near-infrared devices, is emitted as invisible light of a particular wavelength. Initially, early devices emitted 810 nm (nanometer or 10-9 meters wavelength) (ranges from 800 to 820 nm).4 Since then, other devices have been introduced at 940, 980, and 1,064 nm.4 All these wavelengths are highly absorbed by tissues containing the pigment melanin. Additionally, there is significant absorption into the molecule oxyhemoglobin (found in red blood cells). Some lesser absorption occurs into the water in soft tissue by 980 to 1,064 nm.4 Because the thermal action on tissue comes through fiber contact, addition of carbon onto the end of the fiber (initiation) traps some of the photonic energy, which results in more efficient ablation than a plain-ended (uninitiated) fiber.
Concurrent with the action of ablation, there are lesser understood side effects. First, if no blood is released from smaller vessels, the inflammatory reaction to tissue trauma is significantly reduced. Typically, this is observed as little to no redness, swelling, or postoperative pain. The lower powers used in these procedures also stimulate the mitochondria of the affected cells. Stimulation of the mitochondria raises adenosine triphosphate (ATP) production of each remaining cell, which results in faster wound healing.5
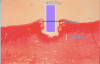
Bottom line: Diode lasers cut by a combination of melting and vaporizing the tissue in contact to a shallow depth. The underlying vascular tissue of the connective tissue does not hemorrhage, due to coagulation of the red blood cells within small vessels. This is perhaps the most important attribute of a diode laser beam (Figure 1).
Conventional Surgical Technique
A scalpel blade has been the usual instrument of choice for the majority of oral surgical procedures. Incisions and excisions are usually performed with scalpels of various sizes and shapes. Advantages include speed of cuts, preservation of the bulk of tissue, and smooth wound edges. However, the disadvantages include the need for complete anesthesia, hemorrhage, postsurgical infection, and a resultant inflammatory postoperative course including redness, swelling, and pain for up to 8 days.6
Laser Surgical Technique
Lasers cut by vaporizing tissue containing a chromophore that absorbs a particular wavelength of the laser light. Simultaneously, a certain depth of coagulation occurs, depending on both wavelength and the power of the beam. The potential speed of the cut is dependent on the wavelength and the power and diameter of the beam. The edges of the wound are more jagged than a scalpel, and a certain volume of tissue is lost to vaporization. Hemorrhage is rare because most lasers can coagulate a blood vessel at least the same size of the employed beam. There is usually no inflammatory response to the surgical intervention, little to no swelling, and reduced postoperative pain. However, overheating the remaining tissue can also cause the inflammatory response to occur due to the thermal damage induced. The wound is concurrently sterilized.6
Perhaps the most beneficial effect is the stimulation of mitochondrial output, mainly ATP and nitric oxide production. The practical results of this include an increase in epithelial cell division and faster healing of laser wounds.
The heat produced during the ablation causes a sterilization of the wound surfaces. There are no known contraindications to the use of a dental diode laser from a medical standpoint.7
Diode Laser Application After Tooth Extraction
The normal healing pattern of a routine extraction would include an expectation of postoperative pain emanating from the gingival collar. When the gingival/periodontal attachment tissue is released from the root before luxation, the inflammatory response begins immediately, initiated by the release of inflammatory mediators from injured cells.
Most practitioners prescribe over-the-counter anti-inflammatory drugs to counteract the tissue effects of the inflammatory process: swelling, redness, and pain.2 Some prescribers have gone beyond this regimen and prescribed opioids as their professional judgment dictates. In the year 2020, practitioners find themselves looking for alternatives to opioids because of the potential for addiction. What are the alternatives? Plant-based topical analgesics? Magic mouthwash? Or nothing? Another method to consider is photobiomodulation.
Photobiomodulation was previously known as low-level laser irradiation. The science behind applying certain wavelengths of light (660 to 1,300 nm) at low power levels (up to 500 milliwatts) for a definitive amount of time directly onto the injured tissue is an emerging therapy.8 Although there are many devices now on the market dedicated to photobiomodulation, a diode surgical laser can be used out of focus (contact) to reduce pain and swelling and even stimulate the healing of wounds.
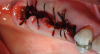
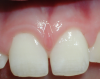
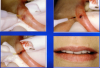
Figure 2 and Figure 3 show a patient who required multiple extractions of posterior teeth. The gingival attachment was elevated, teeth removed, and a diode laser beam (810 nm, 1 watt, continuous wave) applied a few millimeters off the surface onto the inside surface of the reflected tissue for approximately 1 minute per socket before placement of the sutures. The postoperative photograph taken only 3 days later clearly showed advanced healing consistent with the expected appearance 10 days postoperatively. The patient indicated very little postoperative pain and swelling; obviously, there was a reduction in the expected inflammatory response.
Frenectomy
An aberrant muscle attachment extending into the level of the free gingival tissue has negative consequences. The growing child can experience diastema formation directly due to the presence of abnormally positioned attachment fibers. A speech impediment can be caused by an abnormally long lingual frenum. Adults can suffer gingival stripping, loss of tissue height, root exposure, and/or loss of attached gingiva. Any of the above situations may indicate the alteration of these aberrant muscle attachments to prevent or treat the above conditions.9
Conventional surgery with a physical instrument (scalpel, surgical scissors) or electrocautery device involves removing much of the attachment and dissection of the origin/insertion of the fibrous tissue down to alveolar bone. This approach is radical and causes considerable management and postoperative issues. Swelling, pain, constraint of speech, and constraint of eating are among the patient objections to this approach.10
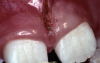
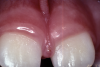
In minimally invasive treatment, a laser procedure is far easier for both the surgeon and the patient. The diode laser is an almost ideal device for labial frenectomy. Minimal local anesthesia is needed. For a thin frenum, a topical anesthetic is often the only necessary anesthetic (Figure 4 through Figure 6).
A frenectomy can be performed with a laser by following the steps below.
Step 1: Only a minimal "wedge" of the frenum should be removed from the center of the frenum, using a hemostat to provide tension on the frenum. The hemostat serves as a "physical surgical guide" to assist in a precision surgical removal.
Step 2: Tension is applied to the lip while selectively ablating any remaining fibers above the periosteum as well as contacting any hemorrhagic vessels.
Step 3: The vestibular fold is deepened 2 to 3 mm apical to the approximal fold. No suturing or surgical dressing is necessary.6
To summarize, advantages of a diode laser frenectomy include the following:
• little to no hemorrhage
• less invasive
• less swelling
• faster healing
• less potential for regrowth or postoperative infection6
Diode Laser Fibroma Removal
The irritation fibroma is the most common tumor-like growth of the oral cavity and represents more than 7% of all biopsy specimens.9 It commonly presents on the tongue, buccal mucosa, and lip. These lesions are raised, and the connective tissue is usually dense and connects to looser connective tissue deeper below the base.
Conventional instrumentation (scalpel) requires careful dissection. Complications include hemorrhage, need to suture the wound, and potential for regrowth due to incomplete removal of the base of the lesion.4
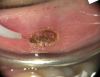
The diode surgical laser can help overcome most of these complications. After a minimum (3 to 4 drops) of local anesthesia is administered surrounding the lesion, the lesions are placed under tension with an instrument (hemostat, tissue forceps) or a suture and pulled away from the adjacent tissue. The diode laser contact tip is then applied along the sides of the lesion and allowed to vaporize the softer attachment fibers of the normal surrounding tissues (Figure 7 through Figure 9).
In summary, advantages of using a laser for fibroma removal include the following:
• no hemorrhage
• less chance of incomplete lesion removal
• no need for suturing the wound (the surface has been coagulated and will heal secondarily quickly)
• little to no swelling and inflammatory response
• faster healing11
Diode Laser Biopsy Acquisition
Abnormal tissue removed from the oral cavity should be examined microscopically and receive a definitive diagnosis. Acquiring the specimen usually requires complete excision with additional normal-appearing tissue surrounding the lesion. Generalists may defer to specialists or ignore the need for acquisitional biopsy, perhaps because traditional instrumentation may cause hemorrhage, requires suturing, and may lead to possible postoperative complications.
The diode laser is an instrument that virtually eliminates the complications of traditional scalpel complications. Hemorrhage during excision is eliminated, with the possible exception of granulomatous lesions. Additionally, the softer connective tissue between the lesion and the fibrous lesion is more easily ablated with a contact laser such as a diode. There is rarely a necessity of postsurgical suturing and postoperative infection.12
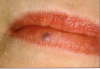
Venous Lake
A common lesion resulting from lip trauma is the venous lake. Before any attempt to treat this lesion, it is imperative to accurately identify it. Although the scope of this article does not include a discussion of the differential diagnosis, it is highly recommended that a differential diagnosis be performed before a decision to treat is attempted.
A standard treatment of venous lake lesion would be to drain the pocket of entrapped venous blood and hope for healing/resolution. However, there is usually a low-pressure supply vessel that refills the vesicle with new venous blood. The key to successful treatment is to prevent this resupply to facilitate healing.
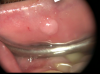
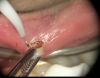
With the use of a diode laser, first the vesicle is opened to allow drainage of the entrapped blood. After that has occurred, the tip of the diode laser is reinserted into the vesicle below the surface and the laser is engaged to cauterize the supply venule. This will occur within a few seconds with a power setting approximating 1 watt on continuous wave mode. The vesicle collapses in the absence of the resupply of blood and heals within 1 week and does not return. The treatment does not cause scarring, which can occur with traditional excisions (Figure 10 and Figure 11).6
Advantages of using a laser in the case of a venous lake include the following:
• procedure takes less than a minute
• little probability of complications
• very fast healing7
Conclusion
Diode lasers can and should become a highly useful adjunct to both a general dental practitioner and surgical specialist. These devices are affordable and relatively simple to use in everyday procedures. Their simplistic approach to many surgical procedures can and should assist practitioners in expanding the breadth of services they provide their patients. The need for training in each specific device cannot be overemphasized. The Academy of Laser Dentistry (laserdentistry.org) conducts unbiased laser training throughout the world. Diode lasers universally replace electrocautery devices without the attending malodor and potential negative sequelae. The use of scalpel and suture should be eliminated for many common surgical procedures in the oral cavity.
The diode laser of today should be considered as the soft-tissue handpiece and a most useful device in everyday care, based on the following factors: hemostasis, ease of use, simplicity of operation, and relatively low cost. Additionally, patients are likely to appreciate lasers and the improvement in postoperative experience.
About the Author
John J. Graeber, DMD, MAGD, MALD, FICD, has been an active general practitioner since 1975 in East Hanover, New Jersey. Dr Graeber is an attending dentist at Morristown Memorial Hospital. He first incorporated diode lasers in 1996 and has been training dentists and hygienists in their use for more than 24 years. He lectures internationally and maintains a diode laser training website, softtouchseminars.com. He has been honored with the Leon Goldman award for clinical excellence by the Academy of Laser Dentistry, where he is a founding member and Past President.
References
1. Food and Drug Administration. 510(k) Premarket notification. https://www.accessdata.fda.gov/scripts/cdrh/cfdocs/cfpmn/pmn.cfm. Accessed February 1, 2020.
2. Manni JG. Basic Aspects of Medical and Dental Lasers. Lulu Publishing Services; 2013.
3. Miserendino LJ, Pick RM. Lasers in Dentistry. Quintessence Publishing; 1995.
4. Moritz A, ed. Oral Laser Application. Batavia, IL: Quintessence Publishing; 2006.
5. Karu T. The Science of Low-Power Laser Therapy. Amsterdam, The Netherlands: Gordon and Breach Science Publishers; 1998.
6. Convissar R. Principles and Practice of Laser Dentistry. Mosby; 2011.
7. Tuner J, Hode L. Laser Therapy: Clinical Practice and Scientific Background. Prima; 2002.
8. Pontinen PJ. Low Level Laser Therapy as a Medical Treatment Modality. Art Urpo Ltd; 1992.
9. Bhaskar SN. Synopsis of Oral Pathology. St. Louis, MO: Mosby; 1973.
10. Newman M, Takei H, Klokkevold P, Carranza F. Carranza's Clinical Periodontology. St. Louis, MO: Saunders, 2006.
11. Olivi G, Margolis FS, Genovese MD. Pediatric Laser Dentistry: A User's Guide. Quintessence Publishing; 2011.
12. Coluzzi DJ, Convissar RA. Atlas of Laser Applications in Dentistry. Quintessence Publishing; 2007.